The SAGE files: Government advisers warned in February that PHE’s contact tracing capacity would be ‘exhausted’ in TWO WEEKS, that there was no evidence for stopping hand-shaking and studies on face masks were ‘weak’ with mixed results
- Government published papers that were presented to SAGE in March/April
- They cover international flights, face masks, social distancing and children
- And showed that scientists agreed contact tracing should be abandoned
Public Health England only had enough contact-tracing capacity to last two weeks before it became ‘exhausted’, scientists warned in February.
Experts said capacity should be increased immediately but admitted it could only be expanded about 10-fold, to contact 8,000 people per day, which still wouldn’t be enough.
A batch of scientific papers submitted to the Government’s SAGE committee were published today and reveal more of what officials were being told in the early stages of the UK’s epidemic.
Researchers said there was ‘no evidence’ that stopping shaking hands would reduce transmission of the virus, shortly after Prime Minister Boris Johnson was ridiculed for continuing to use the greeting.
The papers also showed that there was little evidence in favour of wearing face masks, which have now become mandatory on public transport in Britain.
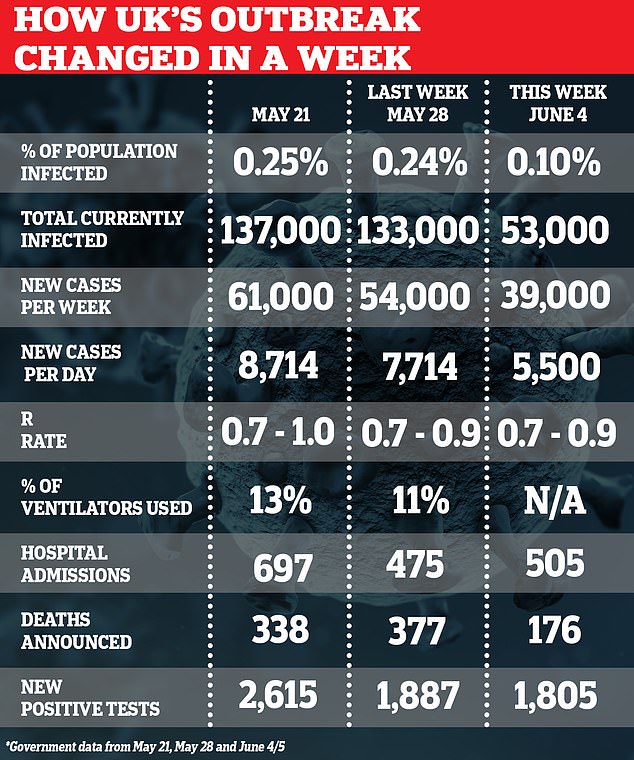
SAGE’s papers have been published as data today revealed that the coronavirus is fading away in England, with only 0.1 per cent of the population now thought to be affected.
This is around 53,000 people, and a drop from an estimated 133,000 in last week’s data. There are now around 5,500 people becoming newly infected each day.
The SAGE papers revealed the following:
- People were already following social distancing before Britain’s lockdown but up to 54 per cent of people in the extra-vulnerable group were not shielding;
- Stopping international flights would not have been a useful measure for the UK during lockdown because there were too many cases already and imported infections would have been drops in an ocean;
- By mid-April there was only ‘weak’ and low-quality evidence that face masks could reduce the transmission of Covid-19 if worn by infected patients;
- People in some settings, such as carers for vulnerable people, may have been better off self-isolating for two weeks. And ‘particular caution’ was urged for discharging people from hospitals to care homes;
- Contact tracing is of ‘limited benefit’ in a large, uncontrolled outbreak and Public Health England’s capacity would have been exhausted within a fortnight;
- Scientists said contact tracing should be stopped when the first case of coronavirus was diagnosed without any clear link to another country or confirmed case;
- Antibody test data – which shows who has had the virus already – should have been available early on in the outbreak to track the size of the epidemic;
- Evidence suggested children under the age of 10 are infected at similar rates to adults but are more likely to have no symptoms;
- Less than 10 per cent of infectious droplets travel further than 5’5″ (1.65m), and transmission at more than 3’2″ (1m) appeared to only be common in hospitals;
- Public Health England modelling predicted that the peak of infections would be towards the end of April if the outbreak was uncontrolled.
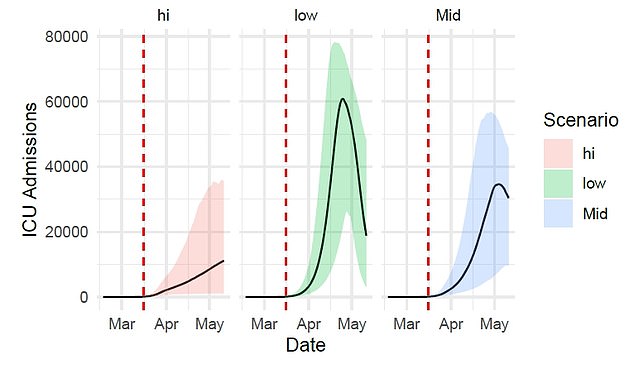
This graph, from a modelling paper produced by Public Health England in March, shows the government organisation predicted that the peak of intensive care admissions would come in late April and stretch up to 60,000 per day if the outbreak was uncontrolled. As it was, the peak was weeks earlier but considerably lower
The SAGE files are now released every Friday as part of a transparency drive by the Government to show the public what advice government officials have been given.
This week’s batch of reports revealed the scientific evidence Whitehall looked at on a number of topics, including international flights, social distancing, face masks, how far the virus travels in the air, when people are most infectious, and how well contact tracing would work.
One of the most damning revelations was that officials were told in February that Public Health England’s contact tracing system would not be enough to cope beyond the very start of an epidemic.
At the time it had the capacity to cope with contacting around 800 people per day, scaleable to 8,000 per day, scientists said.
Contact tracing was brought to an end on March 12 when Professor Chris Whitty, the chief medical officer for England, admitted it was no longer a good use of resources. It has since emerged that this was because too many people had the virus already.
The Government has come under fire for that decision, with other countries like South Korea, which maintained the policy, escaping almost unscathed by the virus.
This is what today’s SAGE papers revealed:
Contact tracing ‘should be discontinued once it is overwhelmed’
A paper sent to SAGE by Public Health England and the universities of Manchester and Cambridge on February 12 warned about the limitations of contact tracing.
A process it called CCI – case and contact isolation – was effective at preventing low-level outbreaks but the capacity in the UK would be quickly overwhelmed if the virus spread out of control.
The researchers said PHE’s capacity – predicted to be good for contacting 800 people per day – should be increased 10-fold at the least.
But it would have to be abandoned when the outbreak spiralled.
The paper warned: ‘Where cases of higher generational numbers become predominant CCI is expected to be of limited benefit outside of certain special cases and should be discontinued.
The current PHE based capacity to provide CCI can be expected to be not sufficient, or sustainable, at the limits of controlling higher rates of incursions into the UK, and should be enhanced…
‘We recommend that CCI should be discontinued when person to person spread is epidemiologically demonstrated to be dominated by second and subsequent generational cases, or, by the contact tracing effort exceeding the management of 8,000 CCI events per day as a proxy.’
Another report suggested that contact tracing should be ended once doctors started to see cases that had no clear links to countries abroad or other confirmed patients.
People were social distancing before lockdown – but not shielding
Survey data presented by the SAGE sub-group SPI-B on March 22, the day before lockdown, found people were already taking many of the measures themselves.
Some 62 per cent of people under the age of 70 said they had already stopped going to pubs, bars and restaurants.
A further 52 per cent said they had stopped going to sports or hobby clubs, because of social distancing advice, along with 30 per cent who were by then working from home.
Half of public transport users had stopped getting buses or trains to try and stop the spread of the virus.
But SPI-B was concerned that between 37 and 54 per cent of the people most at risk from the coronavirus – those who are advised to ‘shield’ themselves – were still meeting up with friends and family.
The report said: ‘Although survey respondents report having stopped or cut down many behaviours, there appears to be room for social distancing to be increased still further.’
Boris Johnson sent the UK into full lockdown the next day, March 23, and urged everyone to stay at home at all times except for essential journeys.
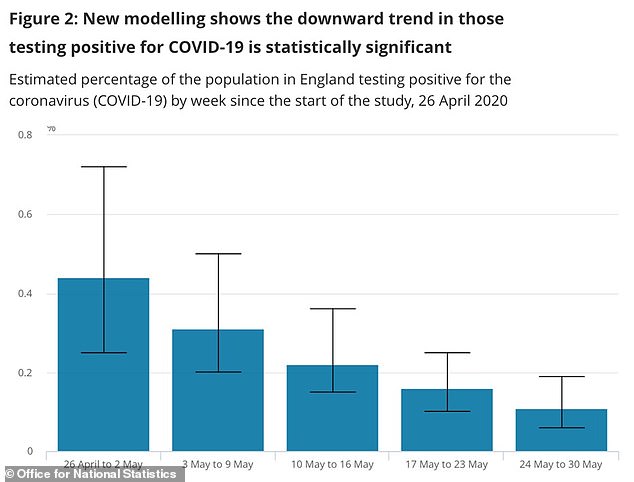
Data from the Office for National Statistics shows a downward trend in the number of people testing positive for the coronavirus over the course of May – from 0.25 per cent at the beginning of May to around 0.1 per cent today
Evidence for face masks as protection was ‘weak’ and mixed
Papers from the first and second weeks of April on the effectiveness of face masks found no clear reason to recommend that British people should wear them.
Researchers noted that scientific studies had had mixed results on their effectiveness and that much of the evidence was not relevant to British society – one had examined how well they worked during pilgrimage.
A paper on April 7 said: ‘Based on the evidence… wearing face mask in the community was not significantly associated with a reduction in episodes of influenza-like illness’.
Scientists quoted a paper that found: ‘Cloth face masks are not as effective as surgical face masks’.
Another paper dated April 13 rowed back slightly but still stopped short of saying face masks should be worn.
It read: ‘There is weak evidence that use of face masks by symptomatic people may reduce transmission.
‘Evidence from randomised trials do not show a protective effect of face masks in community settings but are often affected by low adherence.’
The study suggested the masks could be beneficial if people were likely to cough, because it would catch infectious droplets, but noted that people should be self-isolating if they were unwell.
Face masks were yesterday made mandatory on public transport for people in the UK.
No evidence for stopping hand-shakes, and only 10% of droplets go further than 1.65metres
In a paper dated March 12 scientists discussed how the virus might be transmitted from person to person and looked at hand-shaking and droplet spread in the air.
They found: ‘There is no evidence that avoiding handshakes reduces the risk of infection but on first principles it may result in a minor reduction in risk.’
The paper said that shaking hands was only likely to be a risk if one of the people had the virus on their hands and the other, after shaking their hand, then touched their eyes, nose or mouth.
There were other surfaces people could pick up the virus from and shaking hands did not appear to add any risk, the paper suggested, as long as both people had clean hands.
It added: ‘If people wish to avoid handshakes, it is reasonable.’
The same paper explored how far droplets containing the virus would spread in the air and said only 10 per cent of them made it further than 5’5″ (1.65m) after leaving someone’s mouth.
Social distancing guidelines in the UK are currently to stay 6’6″ (2m) away from others, but shops, cafes and pubs are pushing back to try and get this reduced so they can let customers return.
The SAGE paper said studies of other viruses found almost 90 per cent of droplets from talking alone fell to the ground within 30cm, while for coughing around 15 per cent could travel 50cm.
It concluded: ‘In terms of risk of transmission via close contact in the community, 1 metre is a minimum, 2 metres is precautionary.’
PHE predicted 60,000 per day could need intensive care
Predictions made by Public Health England in March laid bare how government scientists knew the potential devastation the epidemic could cause.
Their calculations predicted that, if social distancing was not successful, the virus could have led to 60,000 people per day needing intensive care at its peak.
In this scenario it predicted the peak would come at the beginning of May and would clearly have been devastating.
Graphs in the report showed 2.5million new infections per day across the country was not outside the realms of possibility, peaking in mid-April.
The peak of infections is actually thought to have arrived in March, owing to the lockdown measures, before a peak in hospital deaths hit on April 8.
The PHE report in March said: ‘Current data on confirmed cases and deaths indicate a possible peak in infections as early as mid April and a corresponding peak in ICU admissions well above current capacity.’
Use ‘particular caution’ when discharging patients to care homes
NERVTAG, one of SAGE’s advisory groups, warned the Government in April that particular care should be taken if discharging hospital patients to care homes.
Officials have come under fire for doing this in the early stages of the outbreak as care bosses accused them of doing it without testing people, and in the process ‘seeding’ devastating outbreaks that killed many residents.
At least 12,500 care home residents are known to have died as a direct result of Covid-19, while many more are thought to have died from indirect effects.
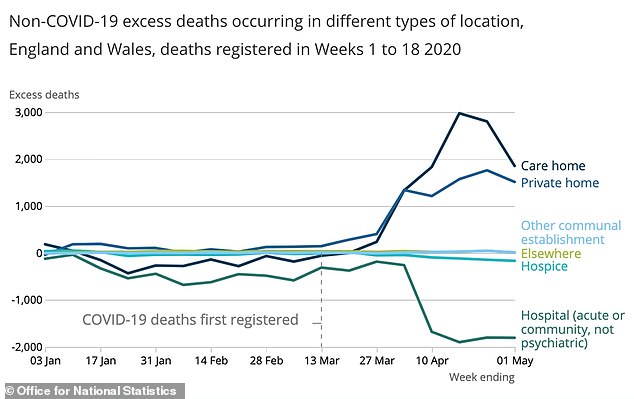
ONS data shows there was a large spike in the number of people dying in care homes in April, the peak of Britain’s coronavirus crisis, as thousands fewer people died in hospitals during that time
NERVTAG’s report was concerning the length of time people should isolate for if they had coronavirus but did not need hospital treatment.
It said seven days was ‘reasonble’ for people with mild illness but others might need longer.
They could include carers, people with weakened immune systems, or more seriously ill patients, who may remain infectious for longer.
The report added: ‘Particular caution should be exercised in Covid-19 patients discharged from hospital to nursing homes, homeless shelters, or other institutions where there are vulnerable individuals.’
An NHS spokesperson said: ‘Guidance of February 24 on discharges to care homes was replaced by further advice from government on March 19, and the NHS has followed all advice from PHE and government, throughout this pandemic.’
Stopping international flights ‘not a useful measure’ in March
In a paper dated March 22, the day before lockdown, scientists said stopping international flights in a bid to stop people bringing the coronavirus to the UK from abroad was ‘not a useful measure’.
There were so many people already infected in Britain that any imported cases would be drops in the ocean, the paper explained.
It said: ‘The initial view from SPI-M is that given the current widescale transmission of COVID-19 within the UK, measures to stop imported cases would have negligible impact. This might change if the UK were to successfully contain the epidemic.’
On the subject of ‘hotspots’ the SPI-M committee suggested that flights from Spain and Iran were probably the highest risk.
Spain because of the sheer number of passengers – there were some 15,000 per day still arriving on weekday flights that week.
And Iran because of the severity of the outbreak there – even though passenger numbers were low, there was a high chance some of them might have the illness.
It said flights from countries like France, Italy and Germany were low-risk because they were going through the same experience as the UK and passenger numbers were already low because of their government and airline restrictions.
Britain did not force flights to stop but told people not to travel abroad. Airlines took it upon themselves to stop most flights when passenger numbers dried up.
Antibody data should be available early in the epidemic
Scientists said data from antibody tests – which test people’s blood to see whether they have had the disease in the past – should be made available as early as possible.
Public Health England and the Office for National Statistics only began publishing this data publicly in May, and it suggests around 8.5 per cent of the population have had coronavirus already.
It took months for officials to get tests available to use and they have been accused of being slow to act in getting antibody tests set up.
But following a flu pandemic in 2009 scientists in Britain had warned that this sort of data was ‘critical to inform important national policy decisions’.
The paper presented to SAGE said: ‘Sero-surveillance is critical to determine population immunity and community infection rates.
‘This data cannot be obtained from other sources and is vital to making modelling predictions of the pandemic.’
In 2011, the paper said, a pandemic preparedness strategy had highlighted the importance of antibody tests and said they were ‘a key surveillance initiative that will be required at the start of any pandemic’.
Children just as likely to catch Covid-19, but fewer have symptoms
An undated paper reporting data from China revealed that children under the age of 10 appeared to catch the coronavirus at the same rate as adults.
But minors were much less likely to show symptoms of Covid-19, or would often have such mild illness that their parents or doctors wouldn’t notice it, the scientists said.
The paper, composed by scientific advisers to the chief medical officer, said: ‘From large datasets in China, it would appear that SARS-CoV-2 affects children and young people at a disproportionately low rate relative to the population.
‘However new data suggests that children under 10 are infected at the same rates as adults, but may be asymptomatic or too mildly infected to come to medical attention.
It added that there was no data on how much children transferred the virus to adults, and they added that the quality of evidence at that point was low.
