Incredible moment patient is woken half-way through brain surgery and ordered to play the VIOLIN as surgeons remove a tumour
- Dagmar Turner, 53, was diagnosed with a large slow growing tumour in 2013
- It grew and became aggressive despite her having radiotherapy
- It was located close to an area that controls the fine movement of her left hand
- She played the violin while having complex brain surgery at King’s College
- It allowed surgeons to identify and therefore avoid the areas needed for playing
- The operation went without a hitch and Mrs Turner is back home playing violin
An incredible video shows a patient playing the violin while surgeons removed a tumour from her brain.
Dagmar Turner, 53, was diagnosed with a large slow growing tumour in 2013 after she suffered a seizure during a symphony.
The mother-of-one had radiotherapy, but the tumour continued to grow until it measured 8cm by 4cm.
It was located in the right frontal lobe of her brain, close to an area that controls the fine movement of her left hand – essential for her musical talent.
She was woken half-way through complex six-hour brain surgery, handed the violin and told to play scales.
The approach allowed surgeons to identify and therefore avoid the areas of the brain that are activated while she plays.
After a successful operation at King’s College Hospital in London, led by Professor Keyoumars Ashkan, in which 90 per cent of the tumour was removed, Mrs Turner is home with her family.
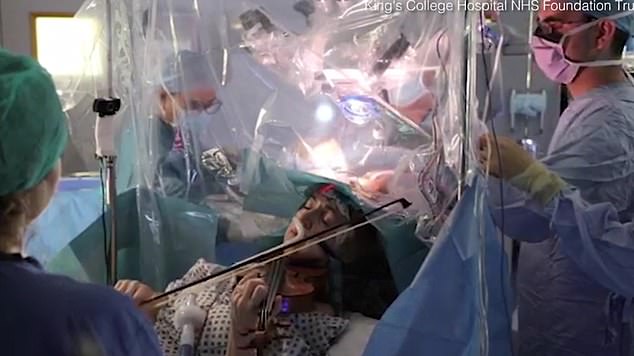
An incredible video shows Dagmar Turner, 53, playing the violin while surgeons at King’s College Hospital removed a tumour from her brain

The mother-of-one was diagnosed with a large slow growing tumour in 2013

Mrs Turner, a musician, was woken half-way through complex six-hour brain surgery, handed the violin and told to play scales. The approach allowed surgeons to identify and therefore avoid the areas of the brain that are activated while she plays
Mrs Turner, a former management consultant from the Isle of Wight, said: ‘The violin is my passion – I’ve been playing since I was 10 years old.
‘The thought of losing my ability to play was heart-breaking but, being a musician himself, Professor Ashkan understood my concerns.
‘He and the team at King’s went out of their way to plan the operation – from mapping my brain to planning the position I needed to be in to play.
‘Thanks to them I’m hoping to be back with my orchestra very soon.’
Mrs Turner, who has a 13-year-old son, was diagnosed with a large grade 2 glioma in 2013.
About a third of brain tumours are gliomas, making them a common type. Low grade means it originated and grew slowly over a period of time.
The musician, who plays in Isle of Wight Symphony Orchestra and various choral societies, had treatment to keep it at bay.
But it kept growing, so she started seriously considering surgery last year.
She explained to her surgeon – who holds a degree in music and is an accomplished pianist – how she was worried she’s lose her skill if she had surgery.
Neurosurgeon Professor Ashkan and the neurosurgical team at King’s devised a plan.
They spent two hours carefully mapping her brain to identify areas that were active when she played the violin.
They also discussed the idea of waking her mid-procedure so she could play.
This would ensure the surgeons did not damage any crucial areas of the brain that controlled Mrs Turner’s delicate hand movements.

Mrs Turner explained to her surgeon – who holds a degree in music and is an accomplished pianist – how she was worried she’s lose her skill if she had surgery

Mrs Turner said she can remember after regaining consciousness, the surgeons just handing her the violin and saying ‘play, play’

Three days after the procedure Mrs Turner was well enough to go home
With her agreement, a team of surgeons, anaesthetists and therapists went on to meticulously plan the procedure.
Professor Keyoumars Ashkan opened Mrs Turner’s skull before she was brought round from the anaesthetic.
Mrs Turner said she can remember the surgeons handing her the violin and saying ‘play, play’ after regaining consciousness.
She was closely monitored by the anaesthetists and a therapist so that the parts of her brain responsible for delicate hand movement and coordination – crucial when playing violin – were not inadvertently damaged during the millimetre-precise procedure.
Following the procedure Professor Ashkan said: ‘We knew how important the violin is to Dagmar so it was vital that we preserved function in the delicate areas of her brain that allowed her to play.
‘We managed to remove over 90 percent of the tumour, including all the areas suspicious of aggressive activity, while retaining full function in her left hand.
‘It was all those finer details of the fine control of the left hand, for example somebody playing the violin, the pressure on the string all those fast movements moving between one string to another. That was what was unusual for us.
‘King’s is one of the largest brain tumour centres in the UK. We perform around 400 resections (tumour removals) each year, which often involves rousing patients to carry out language tests, but this was the first time I’ve had a patient play an instrument.’
Three days after the procedure Mrs Turner was well enough to go home to her husband and son.
